|
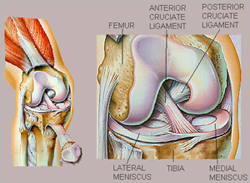
Figure 1. Schematic illustrating the ligaments and the
menisci in the knee. http://arthroscopy.com/sp05001.htm
|
 |
Figure 2. Asa Vaughan, PhD,extruding polymer filaments
that are later braided into artificial scaffolds for ACL and
meniscus reconstruction and regeneration.
|
No tissue repair technology currently exists for large tendon and muscle defects, such as those common to knee injuries, that is natural, strong and large, has good suture retention, and provides enhanced wound healing. The overall goal of this research is the development of suitable scaffolds for the repair/regeneration of the anterior cruciate ligament (ACL) and meniscus (Figure 1). Surgical reconstruction of the ACL using autografts or allografts have been an option for last 30 years. However, problems associated with allografts and autografts such as sterilization, rejection, weakness at the graft donor site, and weakness at the repair site have motivated researchers to develop off-the-shelf alternatives. An engineered scaffold is expected to overcome these disadvantages and potentially provide an ideal substrate for regeneration of natural tissue taking the place of the ACL and meniscus. Our research investigates fibers based on synthetic resorbable polymer, poly(desaminotyrosyl-tyrosine dodecyl dodecanedioate) abbreviated as poly(DTD DD), as one of the potential scaffold materials. This material in conjunction with other promising polymer materials has superior strength, degrades in a tunable manner, will completely resorb via hydrolysis, and has favorable cell compatibility compared to poly-L-lactide (PLLA) fibers. The ACL and meniscus made with poly(DTD DD) fibers in a collagen matrix have been promising in a large animal model.
A secondary goal in this research is the replacement of poly(DTD DD), a polyarylate, with a resorbable polycarbonate. In the design of a polycarbonate scaffold material for the ACL/meniscus, the interchange between retention of mechanical properties and molecular weight degradation is extremely important. Designing the polycarbonate to retain mechanical strength for 6 to 12 months has proven to be very challenging. Any change to the polycarbonate composition inherently changes the mechanical strength, mechanical strength retention time, as well as the degradation profile. Mechanical strength retention for the 6 to 12 months window will allow time for the formation of neoscar tissue and time for the neoscar tissue to become weight bearing within the knee. The neoscar tissue will remain while the polymer scaffold degrades hydrolytically and resorbs into the body. Currently in vitro testing is being conducted on a series of promising polycarbonate formulations.
Project Leader: Asa Vaughan, PhD
Funding Soursce: RESBIO - The National Resource for Polymeric Biomaterials via National Institutes of Health (NIH grant EB001046)

